The other day the insurance of one of our patients wrote to us, claiming that “PRP needling is an experimental and unproven treatment “.
I wrote to them saying that I strong disagree with their opinion and I would be very interested to hear what evidence they could possibly base this statement on.
My own, informed (!), opinion about PRP Needling is not only based on clinical evidence from many, many successfully treated patients here at Eudelo, but also based on scientific evidence from published, peer reviewed, clinical studies.
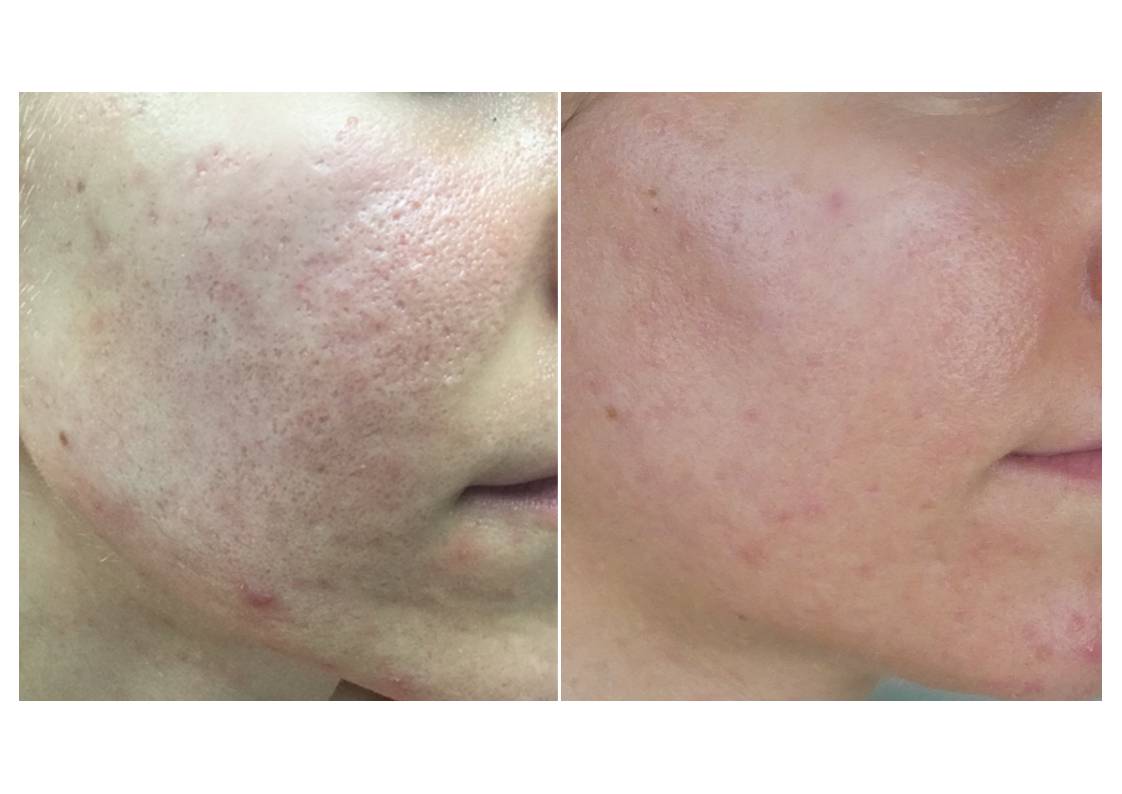
Below I enclosed a selection of examples of clinical studies that clearly demonstrate the effectiveness of PRP needling for acne scaring.
1.) A clinical study published in 2014 for example concludes that RPR needling caused (quote) “HIGHLY SIGNIFICANT IMPROVEMENT IN THE DEGREE OF ACNE SCARS after treatment”. The study also confirmed safety concluding: “No major adverse effects were observed”.
2.) A study published in 2016 confirmed that “PRP has efficacy in the management of atrophic acne scars. It can be combined with microneedling to enhance the final clinical outcomes in comparison with microneedling alone.”
3.) Another study, published in 2018, again confirmed “microneedling in combined with PRP showed satisfactory results”.
4.) I also drew their attention to a review article published in 2017, which concluded that PRP “augments the cosmetic outcomes of microneedling without increasing the risk for adverse events”.
5.) Lastly, I asked them to take notice of yet another study, which again confirmed that “combination between skin needling and platelet-rich plasma is more effective”.
I could go on and on, but I think this little literature review clearly demonstrates that PRP needling is by no means “an experimental and unproven treatment”, as the insurer claimed.
I can only conclude that the insurer has not looked at any scientific evidence for quite a few years.
How very unfortunate with what degree of ignorance we have to deal at times – sigh…
_____________________________________________________________________
1.)
Dermatol Surg. 2014 Aug;40(8):864-73.
Platelet-rich plasma versus CROSS technique with 100% trichloroacetic acid versus combined skin needling and platelet rich plasma in the treatment of atrophic acne scars: a comparative study.
Nofal E1, Helmy A, Nofal A, Alakad R, Nasr M.
Abstract
BACKGROUND:
Platelet-rich plasma (PRP) is an autologous preparation of platelets in concentrated plasma that may be beneficial in the treatment of atrophic acne scars by promoting collagen deposition. Skin needling is a technique that uses a sterile dermaroller to puncture the skin and release growth factors. The combination of skin needling and PRP could enhance the efficacy of both modalities. Chemical reconstruction of skin scars technique consists of focal application of high concentration of trichloroacetic acid (TCA) on the acne scars to stimulate collagen production.
OBJECTIVE:
To evaluate the efficacy and safety of intradermal injection of PRP, 100% focal TCA, and combined skin needling plus topical PRP in the treatment of atrophic acne scars.
PATIENTS AND METHODS:
Forty-five patients with atrophic acne scars were randomly assigned to 3 equal groups; Group A received intradermal injection of PRP, Group B received chemical reconstruction of skin scars technique with TCA 100%, and Group C was treated by combined skin needling and PRP. Each patient underwent 3 sessions at 2-week interval.
RESULTS:
All the patients completed the study. The 3 groups showed statistically highly significant improvement in the degree of acne scars after treatment (p < .001). No major adverse effects were observed in the studied groups.
CONCLUSION:
This is the first study to use intradermal injection of PRP alone for the treatment of atrophic acne scars. The 3 modalities showed a promising efficacy and safety in the treatment of atrophic acne scars.
_____________________________________________________________________
2.)
J Cosmet Dermatol. 2016 Dec;15(4):434-443.
Combined autologous platelet-rich plasma with microneedling verses microneedling with distilled water in the treatment of atrophic acne scars: a concurrent split-face study.
Asif M1, Kanodia S1, Singh K1.
Abstract
BACKGROUND:
Acne scarring causes cosmetic discomfort, depression, low self-esteem and reduced quality of life. Microneedling is an established treatment for scars, although the efficacy of platelet-rich plasma (PRP) has not been explored much.
OBJECTIVE:
The objective of this study was to evaluate the efficacy and safety of platelet-rich plasma (PRP) combined with microneedling for the treatment of atrophic acne scars.
METHODS:
Fifty patients of 17-32 years of age with atrophic acne scars were enrolled. Microneedling was performed on both halves of the face. Intradermal injections as well as topical application of PRP was given on right half of the face, while the left half of the face was treated with intradermal administration of distilled water. Three treatment sessions were given at an interval of 1 month consecutively. Goodman’s Quantitative scale and Quantitative scale were used for the final evaluation of results.
RESULTS:
Right and left halves showed 62.20% and 45.84% improvement, respectively, on Goodman’s Quantitative scale. Goodman’s Qualitative scale showed excellent response in 20 (40%) patients and good response in 30 (60%) patients over right half of the face, while the left half of the face showed excellent response in 5 (10%) patients, good response in 42 (6%) patients and poor response in three patients.
CONCLUSION:
We conclude that PRP has efficacy in the management of atrophic acne scars. It can be combined with microneedling to enhance the final clinical outcomes in comparison with microneedling alone.
_____________________________________________________________________
3.)
J Dermatolog Treat. 2018 May;29(3):281-286.
Skin microneedling plus platelet-rich plasma versus skin microneedling alone in the treatment of atrophic post acne scars: a split face comparative study.
Ibrahim MK1, Ibrahim SM1, Salem AM1.
Abstract
INTRODUCTION:
Acne scarring is a permanent disfiguring sequel, which can take varied morphological forms. Many therapeutic measures have been performed to improve acne scarring such as microneedling. Our objective is to evaluate the efficacy and safety of microneedling alone versus microneedling combined with platelet rich plasma in the treatment of post acne.
METHODS:
The study included 35 patients with mild to severe post acne atrophic scar. All the patients received four sequential treatments of skin microneedling alone on the right side of the face and skin microneedling followed by topical application of platelet rich plasma (PRP) on the left side of the face with an interval of 3 weeks. Two blinded dermatologists evaluated the clinical response according to qualitative global acne scarring system grading of Goodman & Baron. Patients are queried about their satisfaction with the treatment outcomes.
RESULTS:
The study included 35 patients with a mean age of 24.7 ± 6.8 years. There was a significant improvement in the degree of scar severity before and after treatment on both the sides. Regarding patient’s satisfaction grades, there was a significant improvement after both treatment modalities with insignificant differences between both treatment modalities.
CONCLUSIONS:
Both microneedling and microneedling in combined with PRP showed satisfactory results.
_____________________________________________________________________
4.)
Cutis. 2017 Apr;99(4):239-242.
Microneedling therapy with and without platelet-rich plasma.
Hashim PW1, Levy Z1, Cohen JL2, Goldenberg G1.
Abstract
Microneedling therapy is an increasingly popular treatment of several dermatologic conditions. Platelet-rich plasma (PRP) may serve as a valuable adjunct to improve the regenerative effects of treatment. We review the evidence comparing the results of microneedling therapy with and without PRP. Based on the current preliminary literature, PRP appears to augment the cosmetic outcomes of microneedling without increasing the risk for adverse events.
_____________________________________________________________________
5.) J Cosmet Dermatol. 2017 Sep;16(3):388-399.
Therapeutic effect of microneedling and autologous platelet-rich plasma in the treatment of atrophic scars: A randomized study.
Ibrahim ZA1, El-Ashmawy AA1, Shora OA2.
Abstract
BACKGROUND:
New treatments and techniques were being added over the last few years to treat atrophic scars with variable results and adverse effects.
AIM OF THE WORK:
The aim of this study was to evaluate and compare the therapeutic efficacy and safety of microneedling, autologous platelet-rich plasma, and combination of both procedures in the treatment of atrophic scars.
PATIENTS AND METHODS:
This study included 90 patients with atrophic scars and were classified randomly into three groups: I: 28 patients treated with microneedling, one session every 4 weeks; II: 34 patients treated with intradermal injection of platelet-rich plasma, one session every 2 weeks; and III: 28 patients treated with alternative sessions of each microneedling and platelet-rich plasma, 2 weeks between each session, for a maximum of six sessions.
RESULTS:
There was a statistically significant improvement in the appearance of atrophic scars, with reduction in the scores associated with the clinical evaluation scale for atrophic scarring in all groups, but the improvement was more obvious in group III.
CONCLUSIONS:
Although a single treatment may give good results, combination between skin needling and platelet-rich plasma is more effective, safe with less number of sessions in all types of atrophic scars.
_____________________________________________________________________
Whether you have a medical skin condition which needs treatment or simply want to look your very best, our specialised dermatology team will help you achieve the very best result.

