Disorders of the Scalp & Nails
"Diagnosis and treatment of scalp and nail disorders is part of a dermatologist's work. Hair and nail conditions can be caused by a variety of internal and external factors that can be identified and treated by a Dermatologist."
Scalp & Nail Treatments
Diagnosis and treatment of scalp and nail disorders is part of a Dermatologist's work. Hair problems might include patchy or diffuse hair loss, excessive facial hair growth and various skin conditions affecting the scalp such as psoriasis, eczema and seborrhoeic dermatitis. Usually treatment for these can begin with the first appointment. Our Dermatologists also diagnose and treat nail changes which may be due to a variety of internal or external factors.
Hair Loss
The hair growth problems we see most often in clinic are diffuse, hormone-related hair loss (androgenetic alopecia), stress related hair loss (telogen alopecia) and patchy hair loss (alopecia areata).
Androgenetic alopecia: Hormone-related hair loss is a very common and distressing problem that can occur in either sex, but even more so in men. For women, we can do blood tests to assess your hormone levels. Results though, are often normal as in androgenic hair loss; the hair follicles often simply 'over-react' to regular levels of male hormones in everyone's bloodstream.
We offer topical and systemic treatments to help improve hair growth. One of our topical solutions is a prescription strength scalp tincture specially mixed for you by our partner pharmacy. It contains a number of different, highly effective active ingredients to help combat hormonal hair loss and is only available via our Dermatologists.
It's important to know that due to the length of the normal hair growth cycle, it will take at least 2-4 months for any disturbance to respond to treatment. Success takes patience and perseverance.
Telogen alopecia: In some cases, diffuse hair shedding is caused by a 'shock to the system' a few months prior. We call this type of hair loss 'telogen effluvium'. This is a non-scaring, temporary form of hair loss, which will in most cases recover spontaneously after a few months.
It is normal to lose up to 100 hairs each day as a result of the normal hair cycle. In a healthy scalp approximately 85% of the hair follicles are actively growing (so-called anagen phase) and 15% are resting (so-called telogen phase). If there is some shock to the system (think feverish illness, surgery, accident, emotional stress or shock, extreme dieting, excessive travel with jet-lack etc.), as many as 70% of our anagen hair can be pushed into telogen phase, thus reversing the normal ratio. Interestingly, excessive sun exposure may also be the trigger for telogen hair loss, so can not only harm your skin, but also your hair.
Alopecia areata: This patchy hair loss is a common form of hair shedding in both children and adults. It can arise spontaneously or be triggered by stressful life events. Hair loss occurs very suddenly and can be localised with only one or just a few patches, or it can be quite widespread, sometimes even affecting body hair.
The good news is that alopecia areata is not a scaring form of hair loss and in the majority of cases, the hair grows back after some time. We can't predict when this will happen, but we can certainly offer a topical and/or systemic treatment to try and kick-start the process or prevent further spreading.
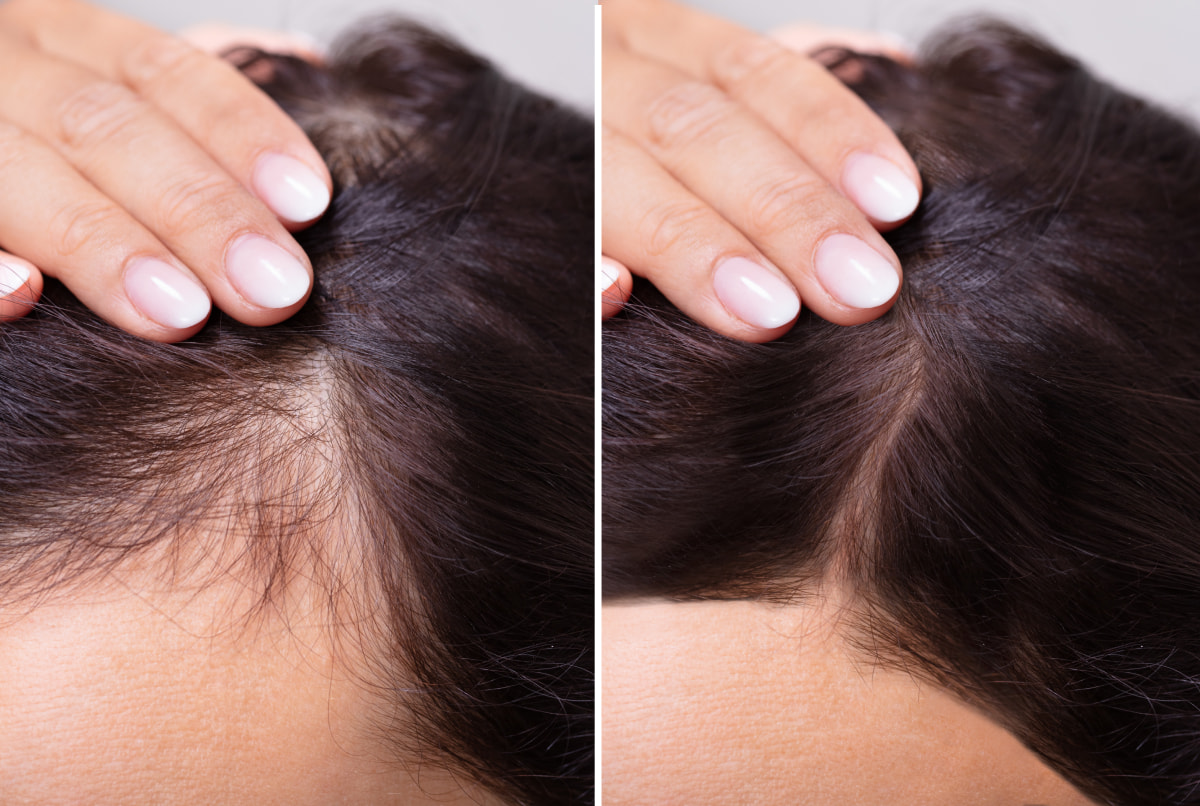
Excessive Facial Hair
In addition to hair loss, our Dermatologists also see patients with excessive facial hair. Again, we might begin with a blood test to rule out any underlying hormonal problem.
Our Dermatologists can prescribe a cream containing eflornithine (Vaniqa®) to slow down facial hair growth. For small areas of unwanted hair (for example on the chin or between the eye brows), one of our Medical Aestheticians can help with a special form of electrolysis called ACP. For bigger areas, laser treatment might be needed. If professional laser hair removal is required, we refer patients to a laser Dermatologist close-by.
Worried About Facial Hair?
Skin Diseases on the Scalp
Certain skin conditions such as psoriasis, eczema or seborrhoeic dermatitis can also affect the scalp skin, causing itching, flaking or scaling, potentially with some hair loss. Scalp skin may also develop fungal infections, which can be highly contagious. Skin conditions on the scalp should always be diagnosed and treated by a Dermatologist.
Nail Problems
Nail changes may be due to fungal infections (onychomycosis), skin diseases such as psoriasis or lichen planus, a deficiency in nutrients such as Zinc, an underlying systemic illness or other reasons.
In clinic our Dermatologist might take nail scrapings for a fungal culture and/or some blood for testing when we begin treatment.
5 reasons to discover Eudelo today
- Specialised and experienced medical dermatology team
Our consultant dermatologists diagnose and treat all skin, hair and nail conditions. - Get a 360° holistic view of your skin’s wellbeing
We look at the underlying causes of your skin condition. - Multi award-winning dermatology clinic
Proven track record of success for diagnosing and treating skin conditions. - Get treatment within the week.
No wait - most appointments can be booked, and treatment started within the week. - Schedule right-now
Our online call booking service means you can take action today.





