Treatments for moles, skin cancer and sun damage
"Skin cancers and moles can be caused by sun damage and the earlier they are detected and treated, the better the outcome for your skin."
Get Your Skin Medically Checked
Skin cancer is a very common type of cancer worldwide and can affect even young people. The good news is that the vast majority of cases are not life-threatening, if detected and treated early. However, if a skin cancer is left to grow untreated, it might not only become more difficult to remove, but could even spread into inner organs, and ultimately shorten your life. That’s why it’s so important to keep an eye on your skin and report any changes to a dermatologist.
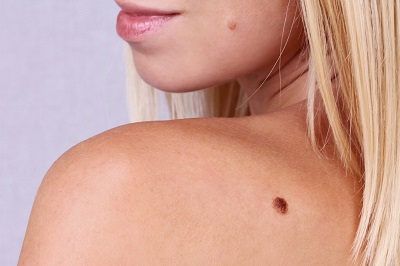
Mole Checks
During your routine check-up, our Dermatologist will inspect your entire body, top to toe (even under the feet and on top of the scalp) to make sure there are no worrying lesions.
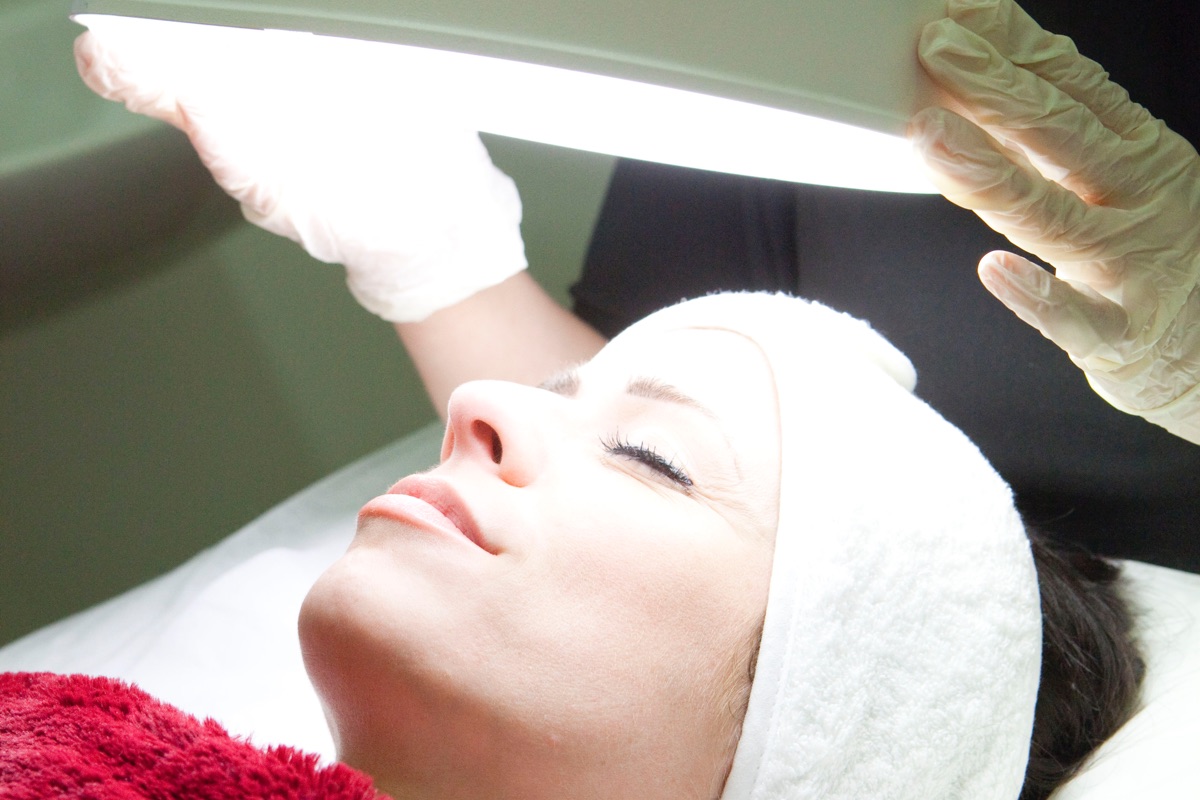
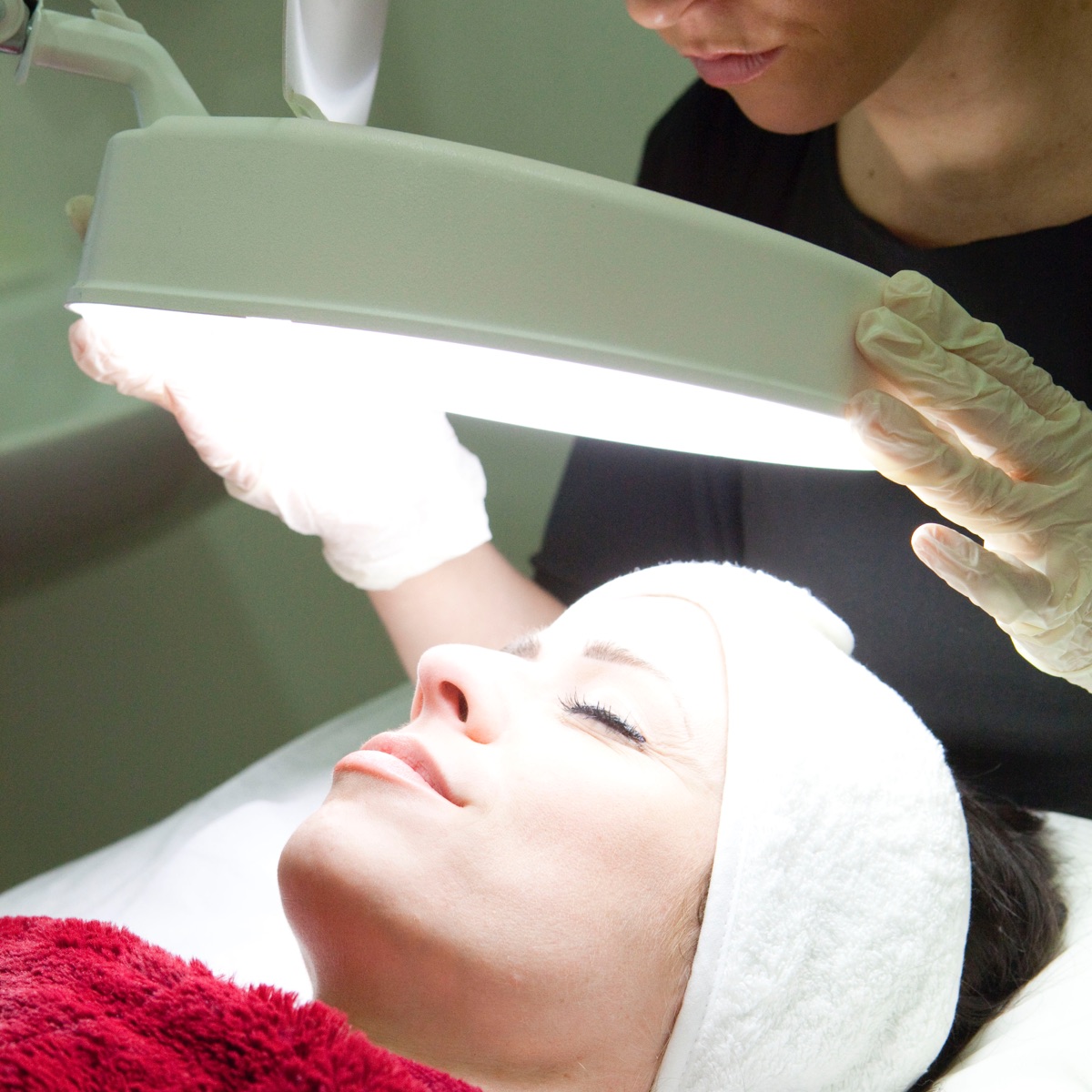
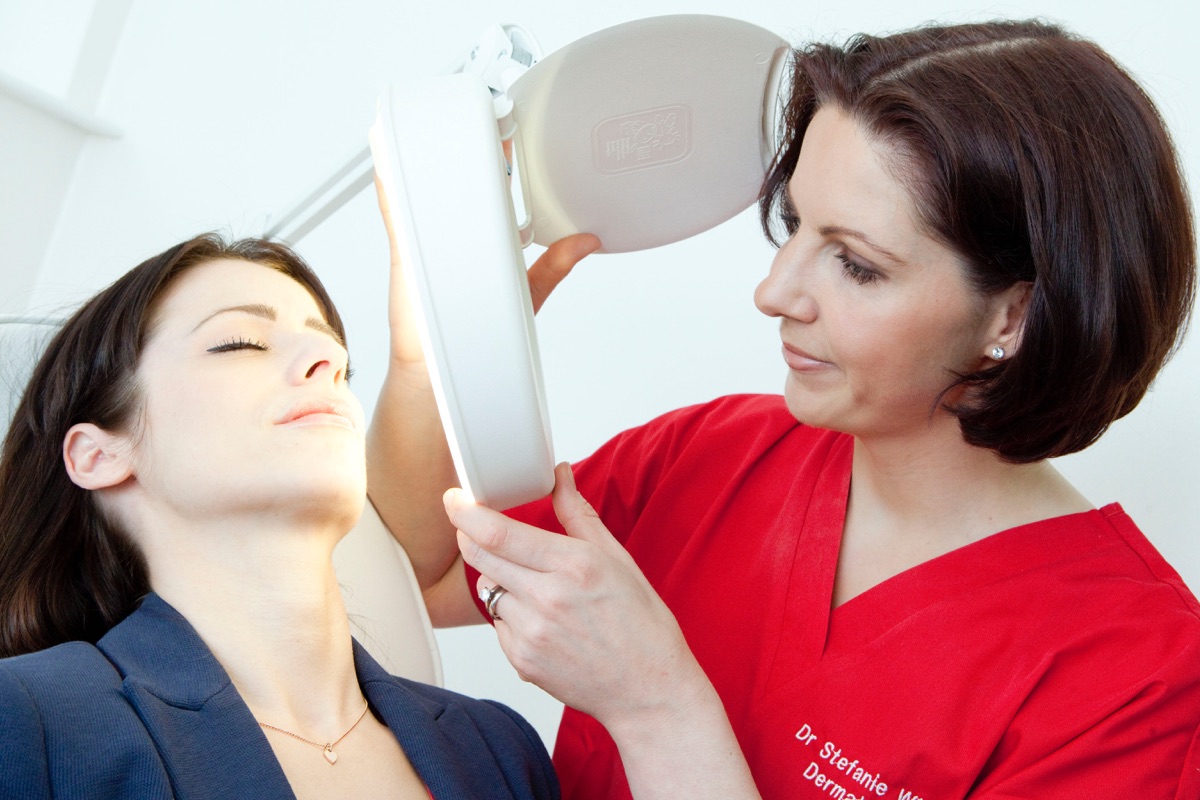
If there is anything remotely suspicious, our Dermatologist will examine the lesion with a dermatoscope, a special magnifying lamp with a polarising light, at no extra cost. Often a diagnosis can be made with this device in a completely non-invasive way.
Moles should not be lasered under any circumstances!
Chronic Sun Damage
A very common problem in the UK is a form of chronic sun damage, known as 'actinic keratoses' (AKs), which often occurs on the face, scalp, hands and forearms. These are in fact pre-cancerous lesions and especially common in fair skin, older people, those who have had quite a bit of sun exposure in the past (through outside hobbies or work, or having lived in a hot country for example).
It might surprise you to hear that your skin 'remembers' every hour of sun right back to your childhood. Once it has 'had enough', it will start to develop pre-cancereous lesions and potentially other problems.
AKs can look slightly red and feel like a patch of rough skin. You might alternatively notice a lesion that keeps on scabbing over. Because AKs are pre-cancereous, it is important to treat them promptly, which can be done by in-clinic 'freezing' (cryotherapy), 'surgical scraping' (curettage) or potent prescription creams.
Worried About Sun Damage?
Skin Cancers
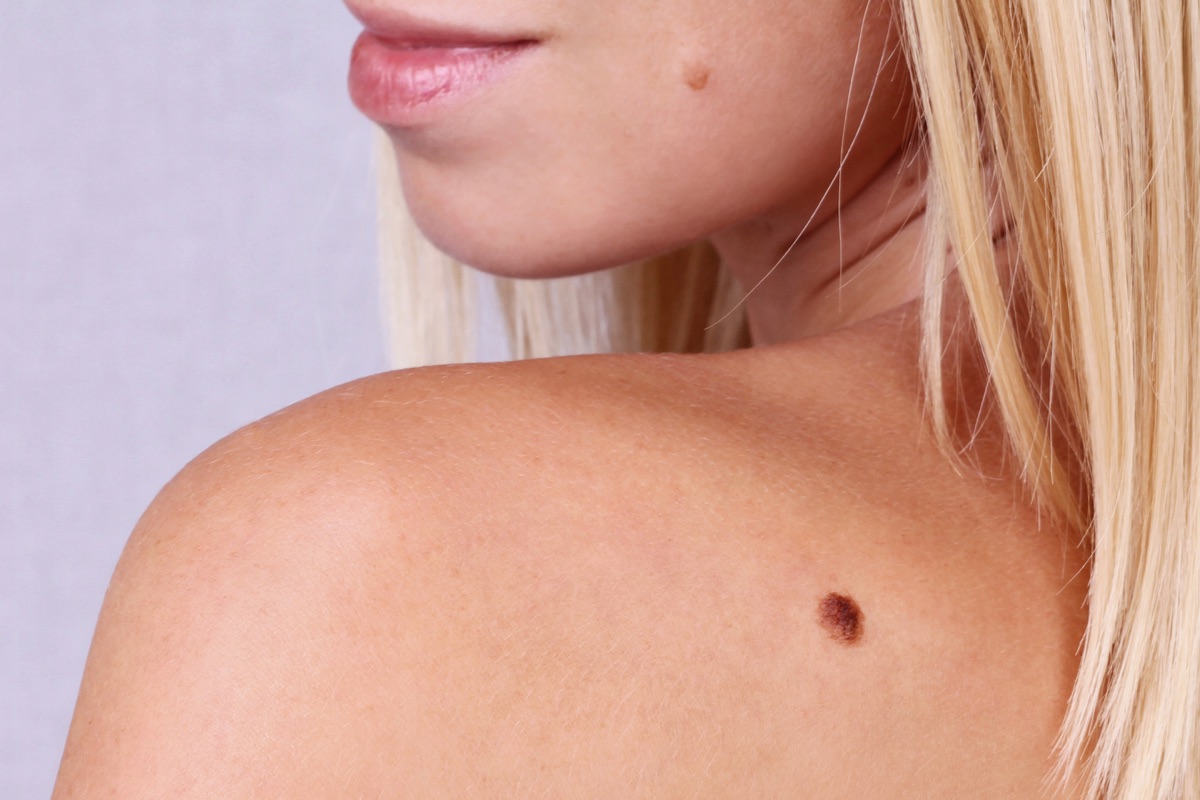
By far the most common type of skin cancer is the so-called 'rodent ulcer' (basal cell carcinoma, BCC). The main cause for this type of skin cancer is past sun exposure and fair skin types are naturally more at risk. The good news about a BCC is that this type of skin cancer does not spread into inner organs and tends not to impact life expectancy. However, if not removed, the BCC will keep growing locally, so an early diagnosis when removal is still straightforward and easy, is extremely important. A basal cell carcinoma can appear in different shapes or forms, such as skin-coloured or pigmented lumps & bumps, ulcerated or bleeding lesions, and scar-like patches.
Other types of skin cancers include squamous cell carcinomas (SCC). But by far the most serious type of skin cancer is a melanoma. This is a malignant skin tumour, which arises from normal skin or in a pre-existing mole. Worryingly, the rate of melanomas in the UK is above the EU average and skin cancer rates in affluent areas are even higher compared to more deprived ones. Overall, cases are rising steeply and, according to the British Association of Dermatologists, the incidence of melanoma is increasing faster than any other common cancer. The good news is that if a melanoma is caught early, the prognosis in most cases will be absolutely fine.
If you notice any changes in a mole (e.g. it becomes larger, changes shape or colour, bleeds or itches) or the development of a new pigmented lesion anywhere on your body, come and see one of our Dermatologists as soon as possible. The lesion will be checked by dermatoscope. You'll be relieved to hear that after the essential clinical and dermoscopic examination, we can reassure the majority of patients. But if a mole remains suspicious, we are able to take it out (which is done painlessly under local anaesthesia) and send the tissue off for special analysis under the microscope.
5 reasons to discover Eudelo today
- Specialised and experienced medical dermatology team
Our consultant dermatologists diagnose and treat all skin, hair and nail conditions. - Get a 360° holistic view of your skin’s wellbeing
We look at the underlying causes of your skin condition. - Multi award-winning dermatology clinic
Proven track record of success for diagnosing and treating skin conditions. - Get treatment within the week.
No wait - most appointments can be booked, and treatment started within the week. - Schedule right-now
Our online call booking service means you can take action today.