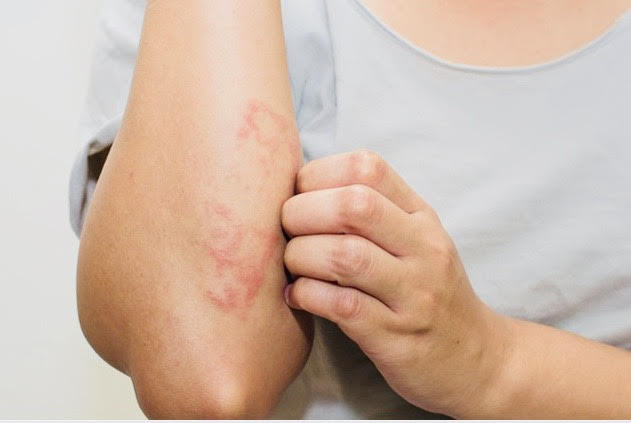
Today is World Eczema Day and with that in mind, I would like to say a few words about eczema in order to raise awareness for this common skin condition.
But before we start, let’s just clarify that when I say ‘eczema’ I mean ‘atopic eczema’. There are of course many different types of eczema including:
- Atopic eczema, the most common type, and the one we commemorate today
- Seborrhoeic dermatitis, which is also common, especially in men (but also babies in the first 4 months of life), but is a completely different condition to atopic eczema
- Contact dermatitis, which is caused by local contact to some sort of trigger,
which can be either irritant (such as for example frequent detergent contact) or allergic (such as for example an allergy to nickel) in nature - Dyshidrotic eczema, a subtype of atopic eczema that comes with tiny, very itchy blisters on the palms and the sides of the finger
- Stasis eczema, a condition on the lower legs, related to chronic venous disease such as varicose veins with swollen ankles and other consequences
- And others….
Also, I should mention that the words ‘eczema’ and ‘dermatitis’ can be pretty much used interchangeably. Sometimes, the word ‘eczema’ is used for more chronic forms and ‘dermatitis’ for more acute forms, but in daily life, most people don’t distinguish these two words.
In any case, from the bullet point list above you can see that there are many different forms of eczema and the first important step is to see a dermatologist get a proper diagnosis, as each form of eczema has its own set of characteristics and treatments.
Today, however, I will be talking about atopic eczema specifically, as this is the most common form and usually what people mean when they talk about ‘eczema’.
Although eczema is a very common skin condition in babies and children (and adults, too, of course), it can be extremely distressing for both child and parent and can make everyday activities and even sleeping very difficult. It’s important to highlight just how debilitating the skin condition can be, and the toll it can take on family life. In fact, AVEENO® Baby undertook research last year which found that 41% of parents believe childhood eczema can impact a child’s quality of life just as much or more than childhood diabetes can and that 1 in 5 parents surveyed felt like they’d failed as a parent because their child had a skin condition.
Let’s find out more about what causes eczema and how to treat it.
What causes eczema?
Atopic eczema is a complex condition that is caused by a number of different factors including the skin having an impaired barrier function (and thus losing excessive amounts of water from the skin, via evaporation, which leads to dryness), an overly reactive inflammatory response and a tendency for allergies.
Atopic eczema is essentially caused by a genetic predisposition for atopic diseases (ie atopic eczema, hay fever, asthma, hives, and other allergies). That means that it is common for eczema (and the other atopic conditions for that matter) to run in families – if one or both parents have some form of the atopic condition, it is more likely that the child will have it, too.
On top of an existing genetic predisposition, certain lifestyle and environmental factors can aggravate the condition, such as detergent contact, the wrong skincare, winter climate, and certain foods such as citrus fruits.
How does eczema present?
Atopic eczema causes the skin to become itchy, dry, thickened, red, cracked, and sore. Some people only have small patches of dry skin, but others may experience widespread areas of inflammation all over the body. Inflamed skin looks red on Caucasian skin and darker brown, purple, or grey on black skin. Very active (acute) eczema may become moist and weep a clear fluid, which should be treated by a doctor asap.
For both children and adults, the condition tends to have (repeated) cycles of flaring up, healing, and then possibly being clear for a while (the latter phase is called remission). The flare-ups can happen either spontaneous (without evident reason) or sometimes due to environmental or lifestyle triggers, such as cold winter weather and/or stress.
Eczema in babies often presents differently from older children and to adults. Key differences include that atopic dermatitis in older children typically affects concave (flexural) body sites such as inner elbows and behind the knees. In contrast to this, babies often develop it on more convex body areas such as the cheeks. In babies, the nappy area is typically free. Adults can either still have the typical flexural sites such as inner elbows and behind the knees affected or may have fewer flexural lesions and more involvement of the head, neck, and hands. Adults also may have more coin-shaped (‘nummular’), lesions rather than the typical bigger plaques in children. However, it’s all very individual, so there is no fixed rule.
Thankfully, most children tend to outgrow eczema before they start school. However, with some children, it can last until puberty when the skin’s oil glands kick in. And in others yet, it will persist into adulthood. And then there are of course some sufferers where the condition only starts in adulthood. We call this ‘late-onset’.
What are the best treatments for eczema?
Treatment for eczema depends on the stage of the skin condition’s cycle. If it is inflamed (flared), it may be that your GP or dermatologist will have to prescribe a steroid cream to stop the inflammation in its tracks. This is important and short courses of topical steroid use are nothing to be worried about. In fact, they are important to prevent complications also, so should not be delayed, when needed.
Alternatively, there are also non-steroidal anti-inflammatory prescription creams such as Elidel® cream and Protopic® ointment that a dermatologist can prescribe.
However, if it is caught early enough (or is in between flare-ups) regular application of emollients (this may be needed multiple times a day!) supports the skin’s barrier function and hydration and maybe all that’s needed.
Remember – even when the skin looks ‘clear’ to the naked eye, i.e. is in remission, it is important to frequently apply emollients to eczema-prone skin in order to lower the frequency and severity of flare-ups.
Also important is the avoidance of irritants such as detergents and soap. A better choice for eczema-prone skin is emollient washes and baths. I also recommend moisturizing directly after bathing, whilst the skin is damp, to lock in moisture.
Can eczema be cured?
Unfortunately, we currently cannot cure eczema, as it is a chronic skin disorder caused by genetic predisposition. It can be managed well though.
A combination of the regular application of emollients; moisturizing baths; avoiding irritants and intermittent use of anti-inflammatory prescription creams from your GP or dermatologist (during flare-ups), can keep symptoms at bay.
Can the sun have an effect on eczema?
Yes, most eczema patients will find the sun helpful to manage their eczema and usually eczema tends to get better in summer and worse in winter. Certain types of UV light are even used in a hospital setting as an effective form of treatment for treatment-resistant cases of eczema.
However, it goes without saying that any sun exposure has to be done very carefully (avoid burning at all costs!) and that cumulative sun exposure will naturally increase the risk of skin cancer, so it’s a double-edged sword.
And while most eczema sufferers will find a moderate amount of sun exposure helpful (there are some patients where the sun makes eczema worse, but that’s an exception), many will find that when it gets too hot and the skin gets sweaty and overheated, this aggravates eczema.
Also, with regards to babies and toddlers, I would like to reiterate not to use the sun as a measure to ‘treat’ their eczema, as young children should not be exposed to direct sunlight for any significant periods until they are at least 2 years old (with or without sunscreen!).
How can I curb my itching?
Scratching eczema can make the condition worse (it’s a vicious cycle) and the skin can become thick and leathery in appearance – this is called lichenification. It is also possible for the skin to become infected from scratching, which can appear as weeping skin with yellow crusts. So, it is important to try and not scratch! I understand though that this is easier said than done…
The most important step to achieve this is of course to see a dermatologist for anti-inflammatory prescription treatment to break the itch-scratch cycle! Prescription creams (and where needed tablets) simply work much stronger than anything available over the counter.
However, there are other measures that can support treatment such as for babies and toddlers cotton or silk gloves or mittens for night-time (you can also get them integrated in PJs), as it’s near impossible to stop a young child from scratching.
Certain types of bandages and/or clothing made from natural fibers such as cotton or silk (but not wool, as this can aggravate eczema!) can also help curb scratching and allow the skin to breathe during.
Also, have a look at ‘wet wrapping’ online – you will find a lot of useful information on this technique and many patients find it helpful for their children with eczema.
Another simple trick can be to keep nails short in order to limit skin damage, irritation, and risk of infection from scratching.
For older children, try to teach them to scratch with their knuckles (tuck the thumb under and fold the fingers over the thumb, then scratch with the knuckles), as opposed to their fingernails. In doing so, it empowers them to scratch in a less damaging manner and it works surprisingly well in my experience.
Lastly, make sure to regularly apply emollients throughout the day to soothe the skin. Some contain anti-itchy ingredients, too. One word of caution about Dermol lotion though. While it’s great as an anti-itch bath or shower additive, it can be irritating when left on the skin, so I don’t usually recommend it as a leave-on product. I also recommend avoiding traditional Aqueous cream as a moisturizer. Aqueous cream was originally developed as a soap substitute and can irritate the skin when used as a leave-on product.
In the summer, you could keep your emollients in the fridge to refresh the skin and calm itchiness for a little while (but don’t do this for babies).
Can eczema be controlled with diet?
Some evidence suggests that eating oily fish or taking fish oil supplements, can help prevent eczema to some extent. There is also some evidence that suggests probiotics can help to not only aid digestion, the immune system, and other body functions, but also reduce eczema.
For Mums, there is also evidence that baby eczema may be reduced by exclusive breastfeeding for a full 4 months, as well as taking probiotics and fish oil supplements throughout pregnancy.
Sometimes eczema gets worse after eating certain foods. This may be an allergy (eg to cow’s milk) or an intolerance (eg to citrus fruit). However, there is no silver bullet and most dietary changes may only show marginal benefits, if at all.
Unfortunately, the only reliable lab testing is for true allergies (which are comparably uncommon).
What should you do if your eczema worsens?
Once you have tried over-the-counter emollients for a week or so without avail, it may be time to head to the GP or dermatologist for a prescription cream.
However, if weeping and/or yellow crusts appear, this could be a sign of secondary bacterial infection and you should see your doctor for consideration of antibiotics asap.
Lastly, if you, or your child, suddenly develop a widespread rash of tiny blisters and sores, this maybe herpetic eczema (i.e. ‘cold sores’ on top of your eczema) and you need to go to the doctors urgently. This type of eczema needs to be treated quickly with anti-viral medication.
I hope this educational content was helpful. Please feel free to share.
And if you need help with your eczema, we have six dermatologists at Eudelo who are more than happy to help. Three of them also specialize in pediatric dermatology.
Yours,
Dr Stefanie
Whether you have a medical skin condition which needs treatment or simply want to look your very best, our specialised dermatology team will help you achieve the very best result.

